View Other Articles
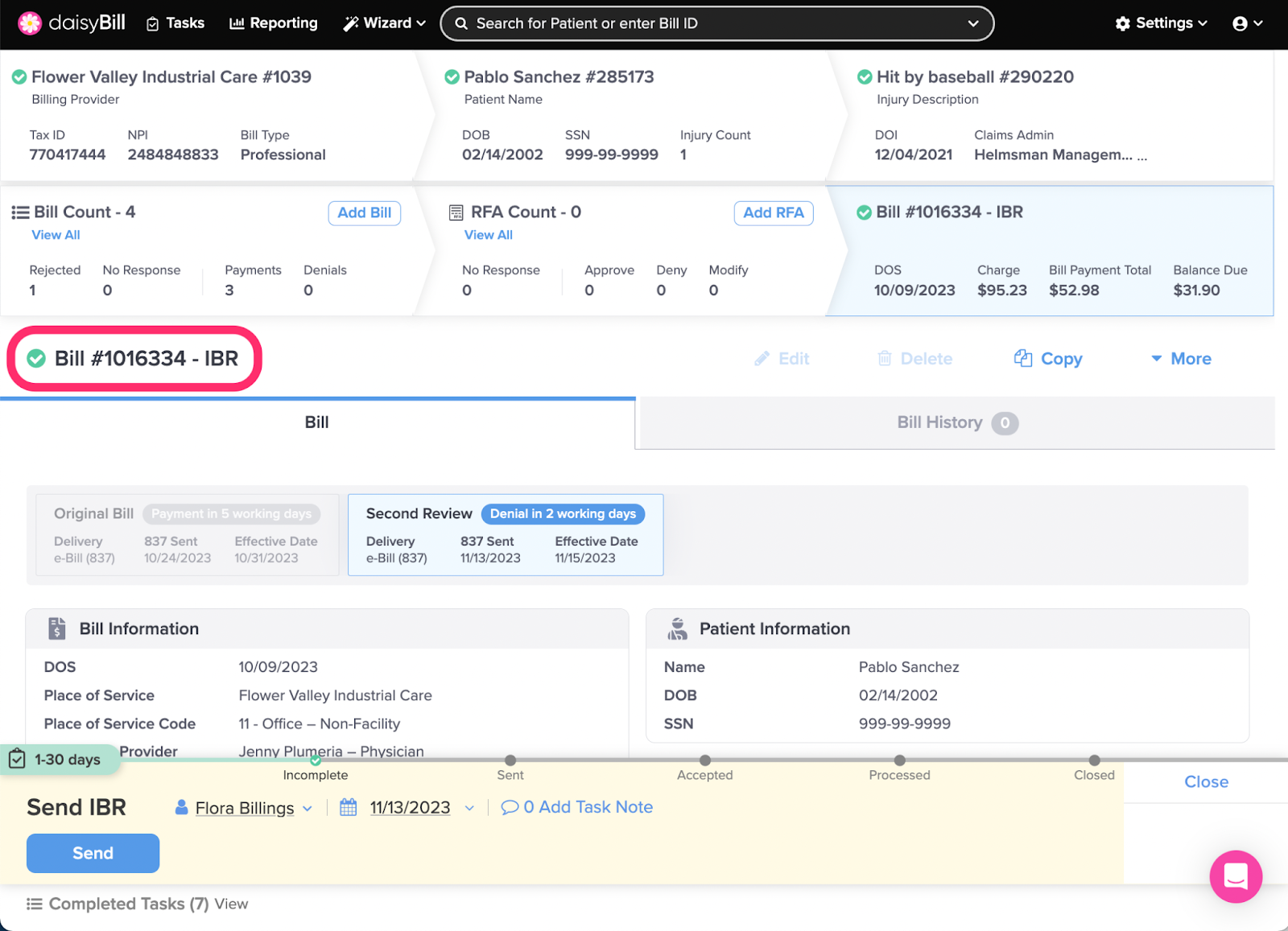
A Bill in Independent Bill Review status indicates a user at your practice determined additional reimbursement is due, because the claims administrator incorrectly processed the Second Review.
When completing either the Payment Received - SBR or Denial Received - SBR task, the daisyBill user determined both that:
- Additional reimbursement remains due for the bill, and
- Independent Bill Review (IBR) is the appropriate method to collect additional outstanding reimbursement (as opposed to filing a lien).
Associated Tasks
Next Steps - Within 30 Days of Second Review EOR
- Review § 9792.5.7. Requesting Independent Bill Review.
- Create the IBR Submission in DaisyBill
- Pay the current $180 IBR Fee
That’s it!