When a $0 reimbursement is posted to an Original Bill submission, daisyBill automatically moves the Bill to Processed status, generates a Denial EOR task, and assigns the task to a designated daisyBiller.
To complete the Denial EOR task determine whether additional funds remain due for the bill.
Watch Denial EOR tasks closely. For incorrect reimbursements, timely completion of Denial EOR tasks guarantees submission of Second Bill Reviews (SBRs) within the mandated 90-day timeline.
Here’s how it’s done.
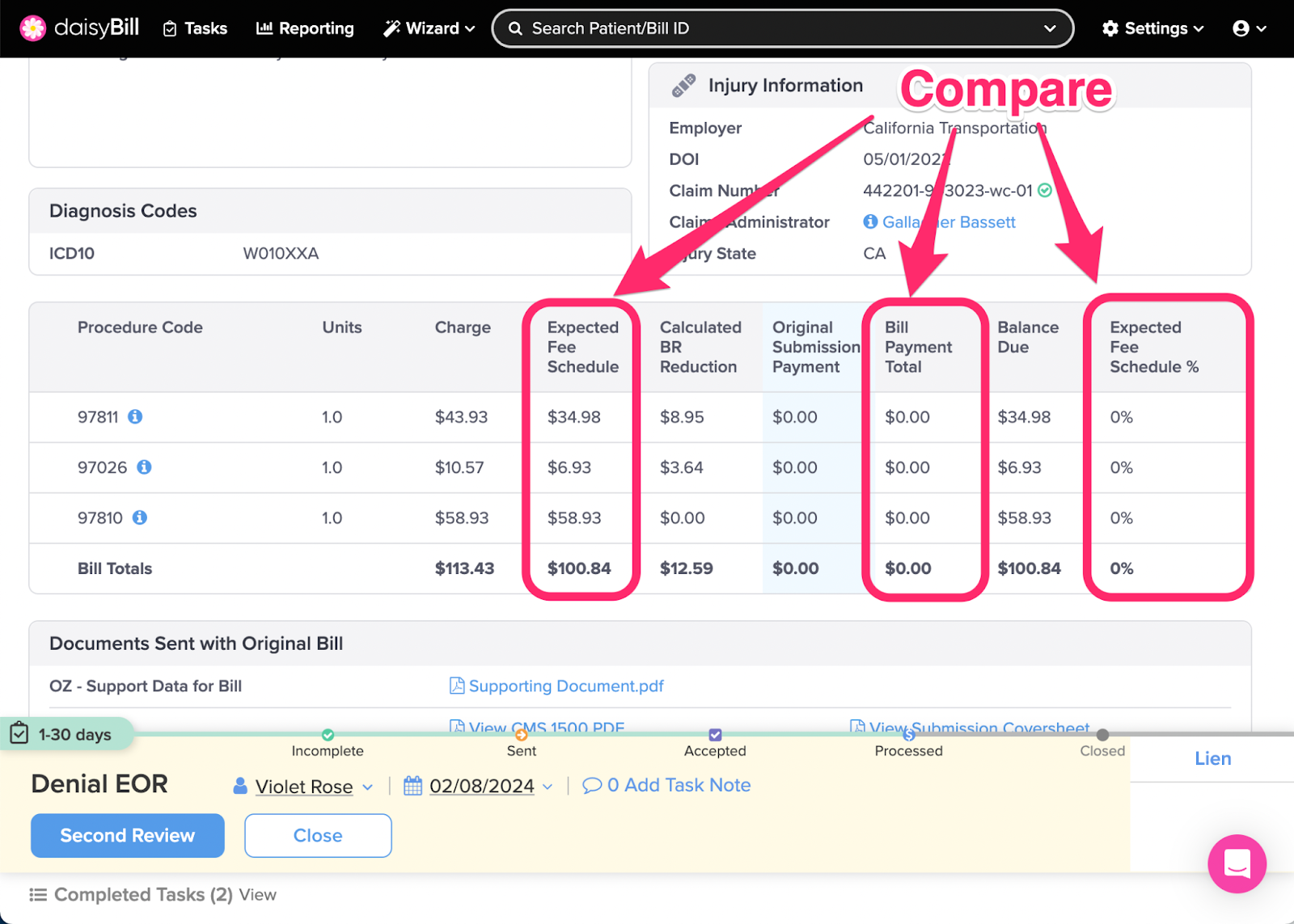
Step 1. For each Procedure Code, compare the ‘Expected Fee Schedule’ amount to the ‘Bill Payment Total’
Expected Fee Schedule: daisyBill calculation of state fee schedule (for supported states), or, Organization's set Expected Reimbursement.
Bill Payment Total: Total of all payments posted to all submissions of the bill.
Expected Fee Schedule %: Bill Payment Total divided by Expected Fee Schedule.
Balance Due: Expected Fee Schedule less Bill Payment Total.
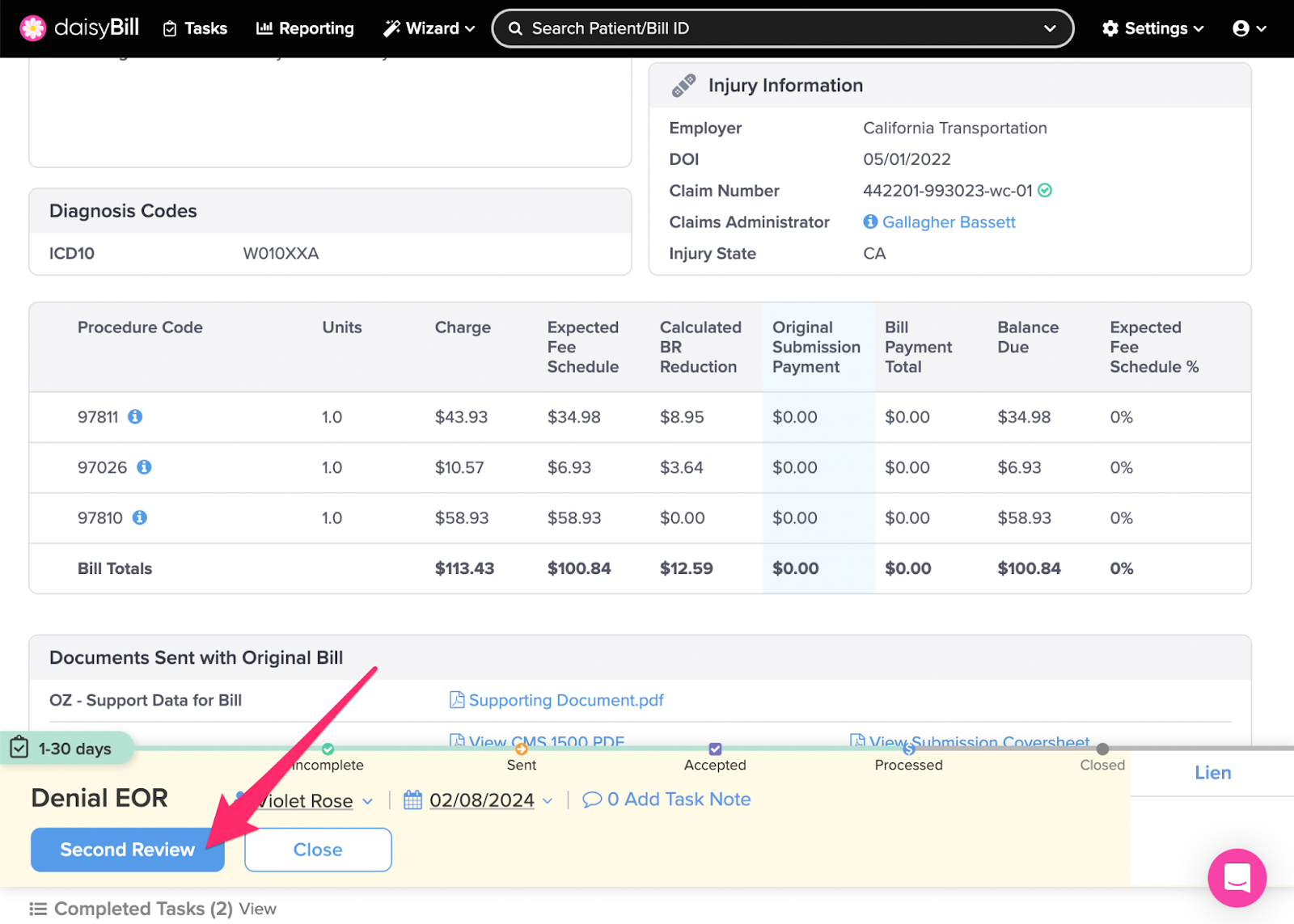
Step 2. For insufficient payments, choose an option from the ‘Action Bar’
Second Review: Changes Bill Status to Incomplete, navigates to the Second Bill Review (SBR) functionality. For more information, see the Help Article: Request for Second Review: Denied Bill.
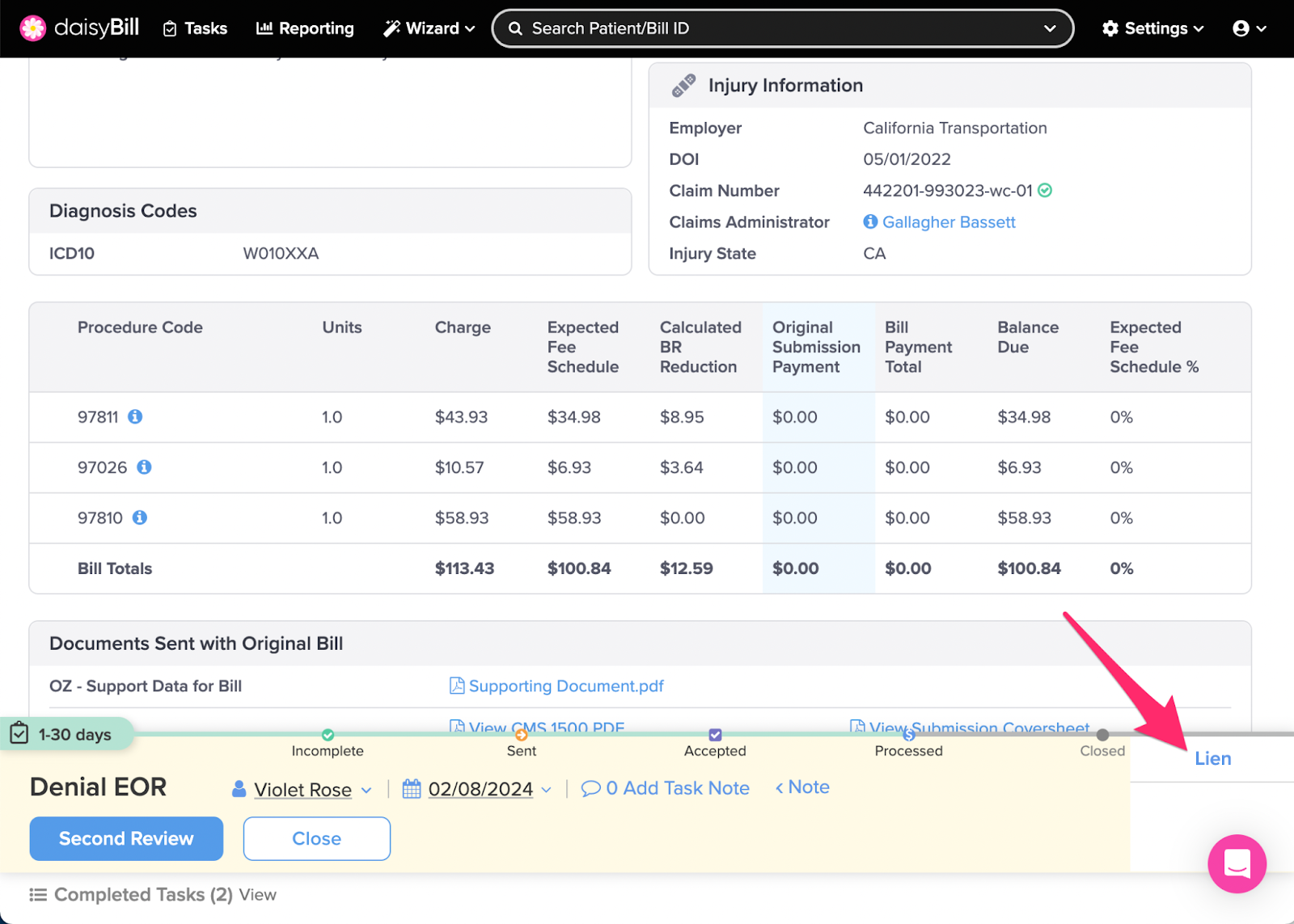
Lien: Changes Bill Status to Lien, queues the bill with all other bills for the injury marked for Lien status. (But does not file a lien. This must be done outside daisyBill.) For more information, see the Help Article: Mark Bill as Lien - Lien Filed.
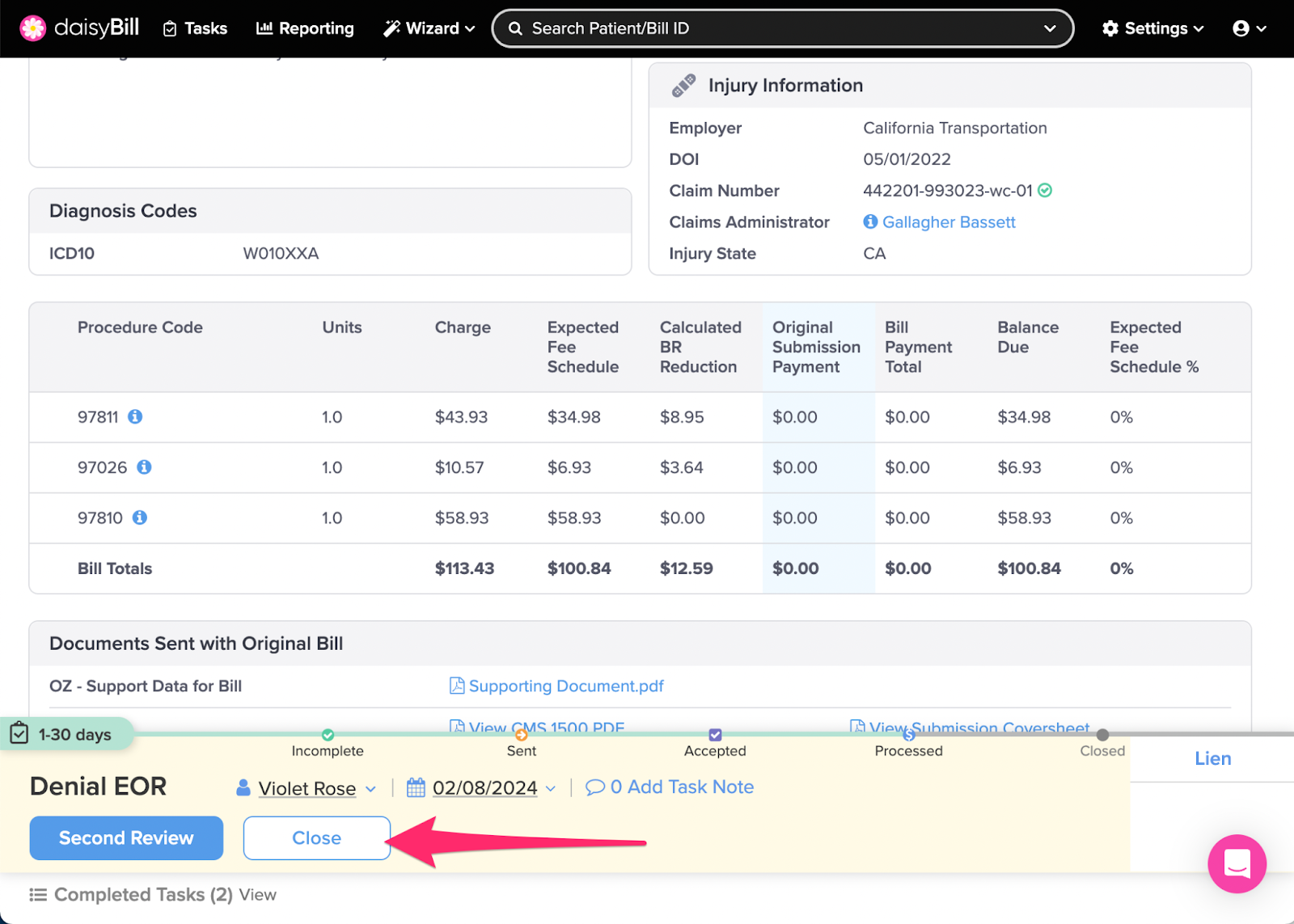
Step 3. For sufficient payments, click ‘Close’
This moves the Bill to Closed status and completes the task.
Nice work!