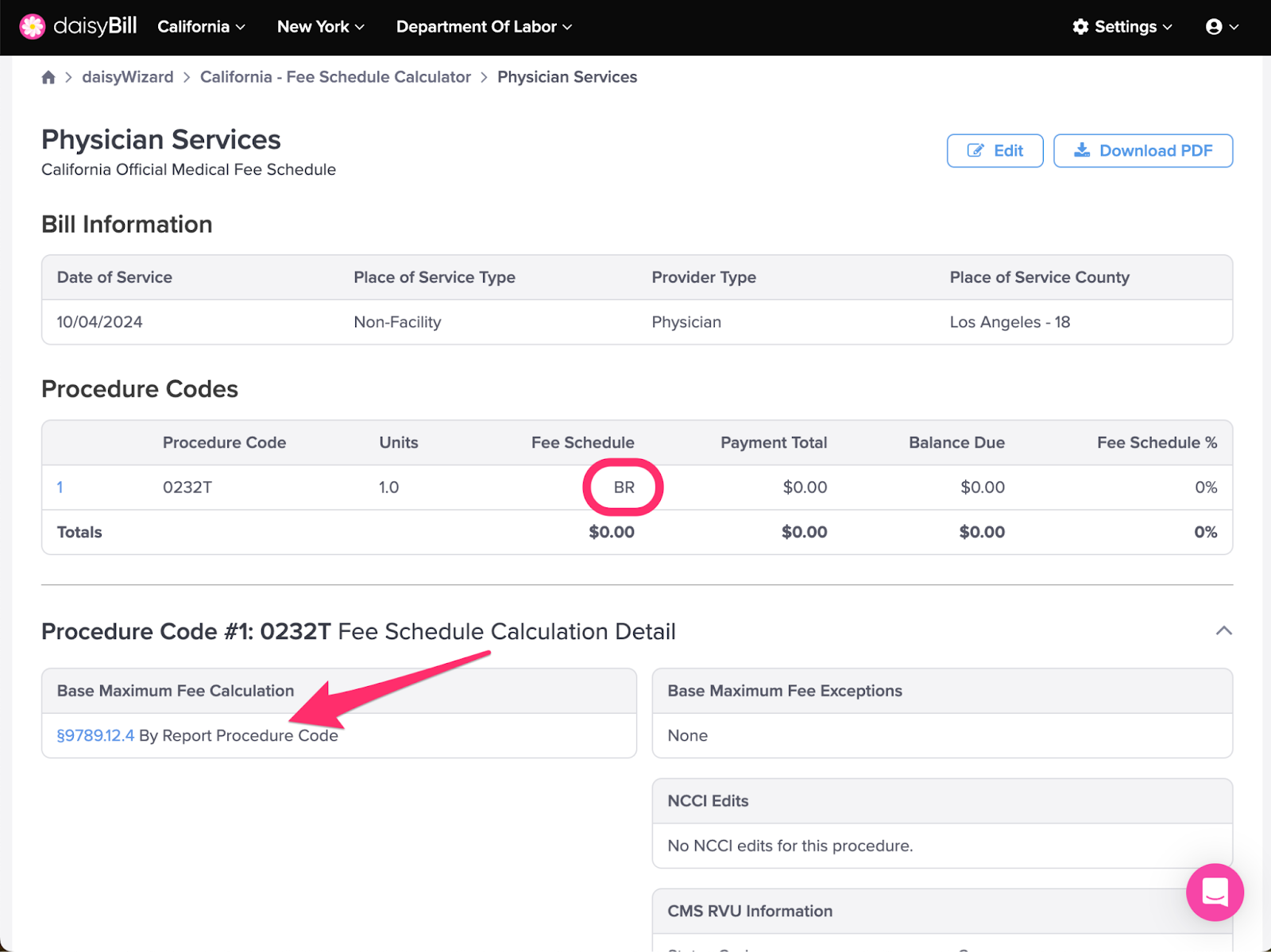
The display of ‘BR’ in the OMFS reimbursement field indicates that the reimbursement amount for the Procedure Code is determined ‘By Report’ (BR).
A. ‘By Report’ (BR) Reimbursement Value
B. Required ‘By Report’ (BR) Documentation
C. Unlisted Procedure Codes / Procedures Lacking RBRVUs
D. Independent Billing Review Final Determinations
A. ‘By Report’ (BR) reimbursement value
When the OMFS Calculator displays BR in the OMFS column, it means the Procedure Code is reimbursed on a By Report basis. BR Procedure Codes are valid billing codes but do not have a Base Maximum Fee. Accordingly, the provider may bill any value deemed reasonable for the code.
The Physician Fee Schedule regulation states that when determining the reimbursement value of the BR Code, “consideration may be given to the value assigned to a comparable procedure or analogous code. The comparable procedure or analogous code should reflect similar amount of resources, such as practice expense, time, complexity, expertise, etc. as required for the procedure performed.” § 9789.12.4. “By Report” - Reimbursement for Unlisted Procedures/Procedures Lacking RBRVUs.
B. Required ‘By Report’ (BR) documentation
When billing a BR Procedure Code the Physician Fee Schedule regulation requires an accompanying report (report not separately reimbursable) which should include:
“the service was reasonable and necessary to cure or relieve from the effects of the industrial injury or illness. Pertinent information should include an adequate definition or description of the nature, extent, and need for the procedure, and the time, effort and equipment necessary to provide the service.” § 9789.12.4. “By Report” - Reimbursement for Unlisted Procedures/Procedures Lacking RBRVUs.
C. Unlisted procedure codes / procedures codes lacking RBRVUs
A Procedure Code is deemed By Report (BR) for one of four reasons:
- Unlisted procedure code as listed in the Current Procedural Terminology (CPT) codes. Reimbursement is designated as ‘By Report’. CCR. § 9789.12.4. “By Report” - Reimbursement for Unlisted Procedures/Procedures Lacking RBRVUs.
- Procedure codes with status indicator codes C, N, I or R that do have RVUs assigned under the CMS' National Physician Fee Schedule Relative Value File, these procedures codes are billed as ‘By Report’. CCR § 9789.12.3. Status Codes C, I, N and R.
- Procedure codes with status indicator E are billed as ‘By Report’ that: 1) do not start with ‘J’ or ‘P’, and 2) fee schedules Section 9789.30-9789.70 are not applicable. CCR § 9789.12.8. Status Codes.
- Procedure codes with a status indicator code X are billed ‘By Report’ only when the fee schedules Section 9789.30-9789.70 are not applicable. CCR § 9789.12.8. Status Codes.
D. Independent Bill Review (IBR) final determinations
IBR Decisions make excellent Supporting Documentation for Second Reviews for BR Procedure Codes.
Below are examples of Independent Billing Review Final Determinations that pertain to BR codes. These Decisions have been ruled on by Maximus and are available publicly on the DWC website.
- http://www.dir.ca.gov/dwc/IBR/IBR-Decisions/Decisions2015/IBR2015_601-900/CB15-0000806.pdf
- http://www.dir.ca.gov/dwc/IBR/IBR-Decisions/Decisions2015/IBR2015_101-300/CB15-0000121.pdf
- http://www.dir.ca.gov/dwc/IBR/IBR-Decisions/Decisions2015/IBR2015_901-1200/CB15-0001125.pdf
- http://www.dir.ca.gov/dwc/IBR/IBR-Decisions/Decisions2015/IBR2015_301-600/CB15-0000341.pdf
- http://www.dir.ca.gov/dwc/IBR/IBR-Decisions/Decisions2015/IBR2015_10-100/CB15-0000013.pdf