When reimbursement remains due on a bill after Second Review, file for Independent Bill Review (IBR).
Per CCR § 9792.5.7, “If the provider further contests the amount of payment made by the claims administrator on a bill for medical treatment, services, or goods...the provider shall request an independent bill review.”
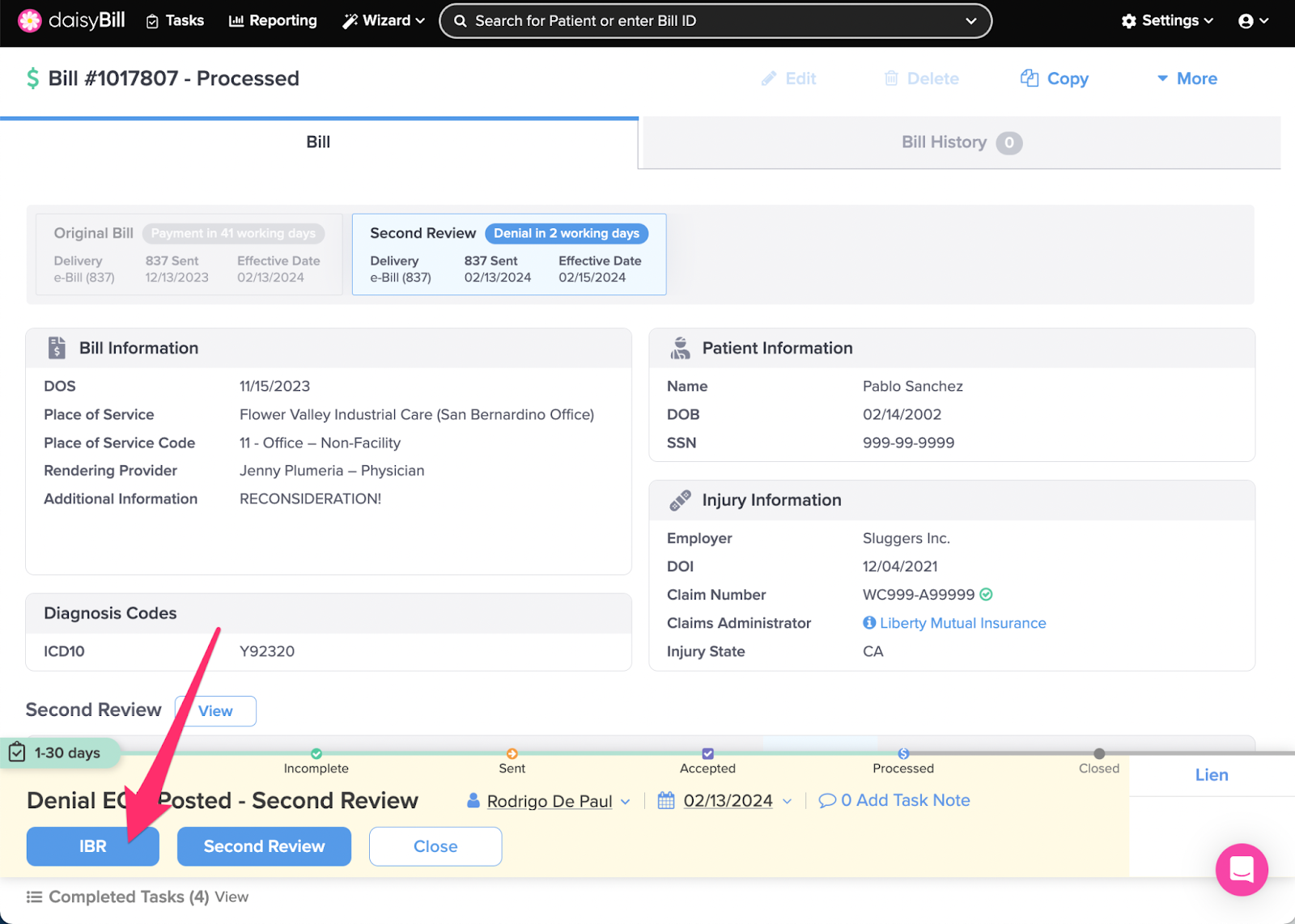
Step 1. Click ‘IBR’
For the IBR option to appear, the Bill must have been sent for Second Review and a Second Review EOR must have been received and posted.
Note: If the claims administrator failed to issue a Second Review EOR within 14 days of receiving the SBR, you can file for IBR. See this Help article for details.
Step 2. Select Procedure Codes to IBR
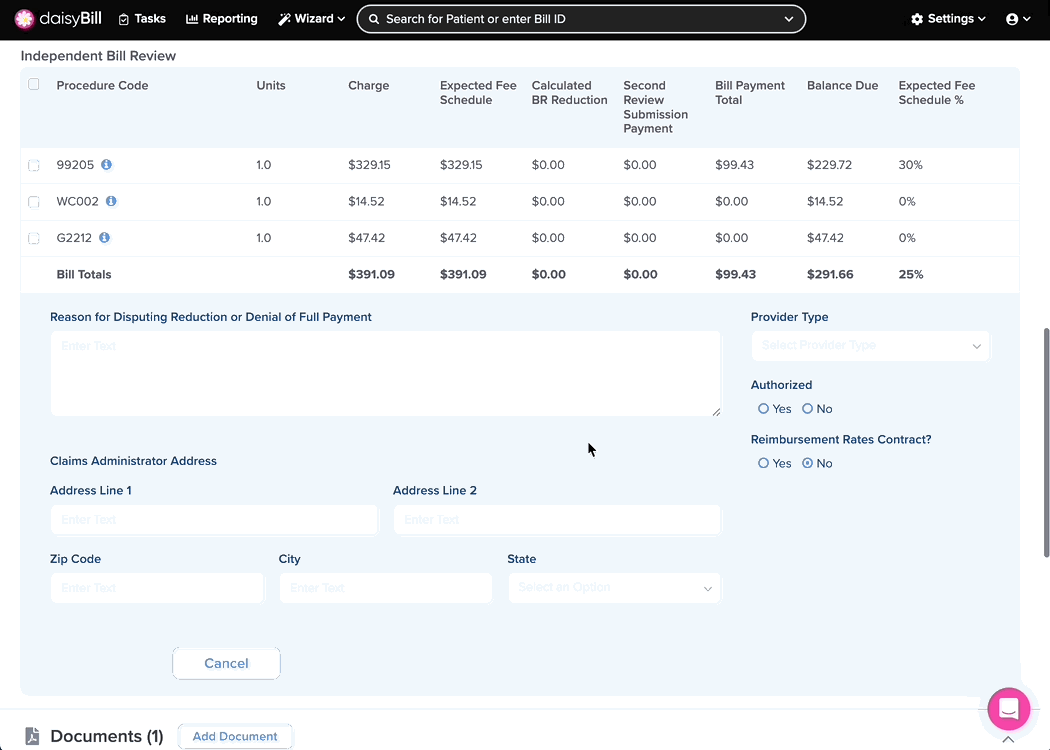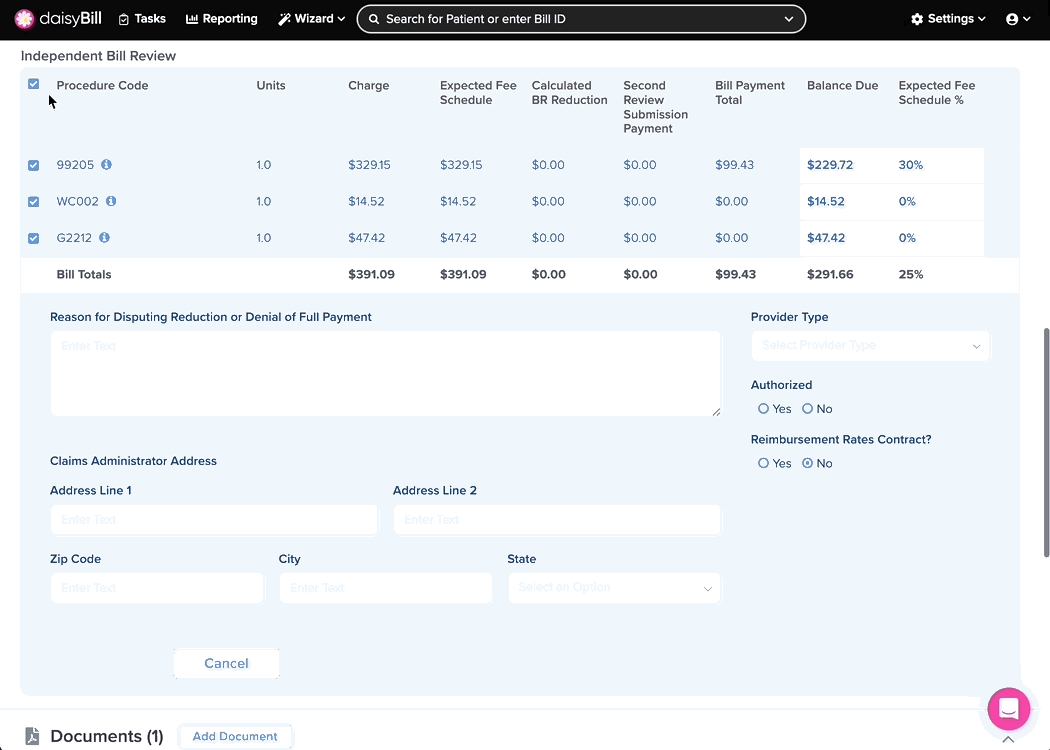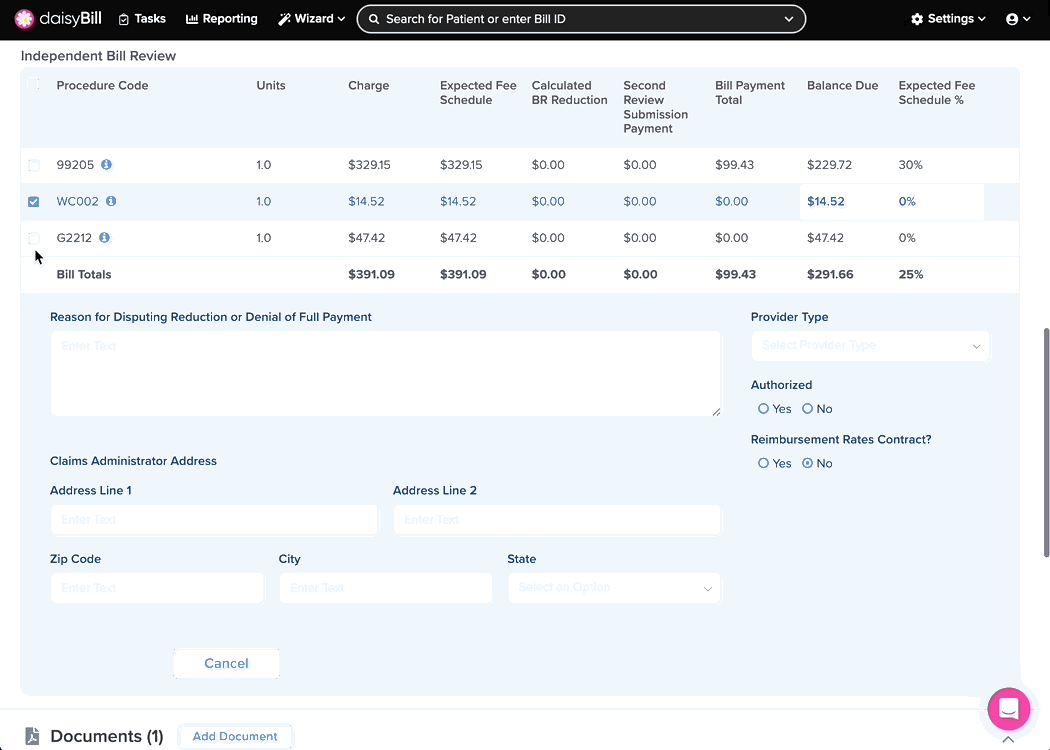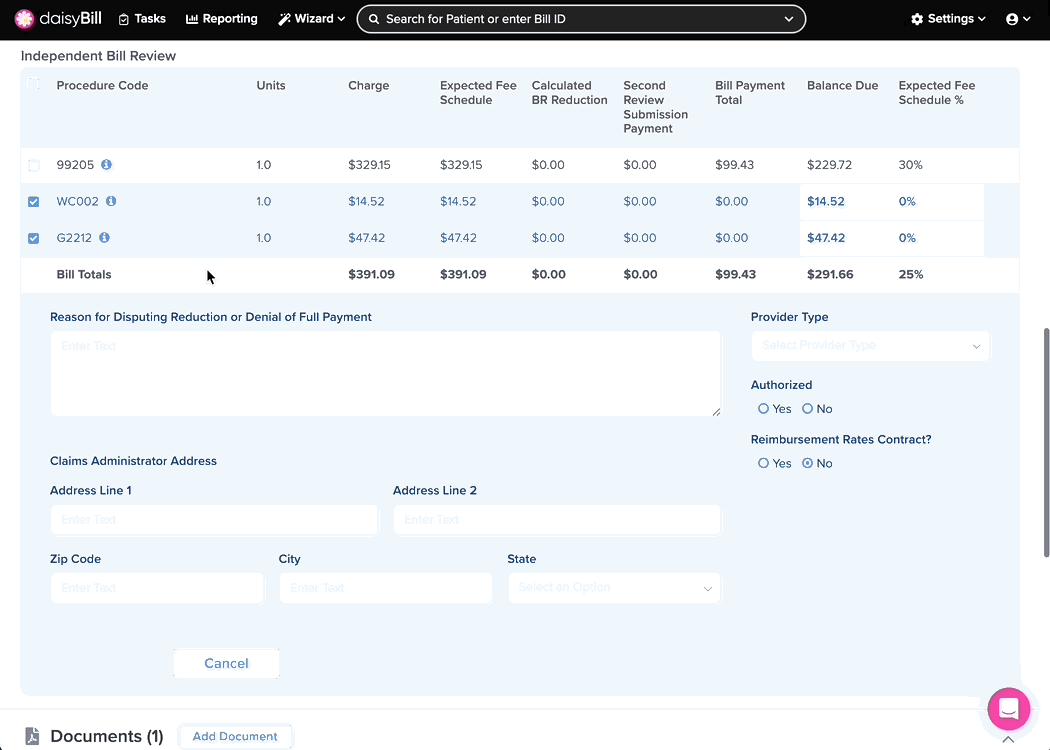
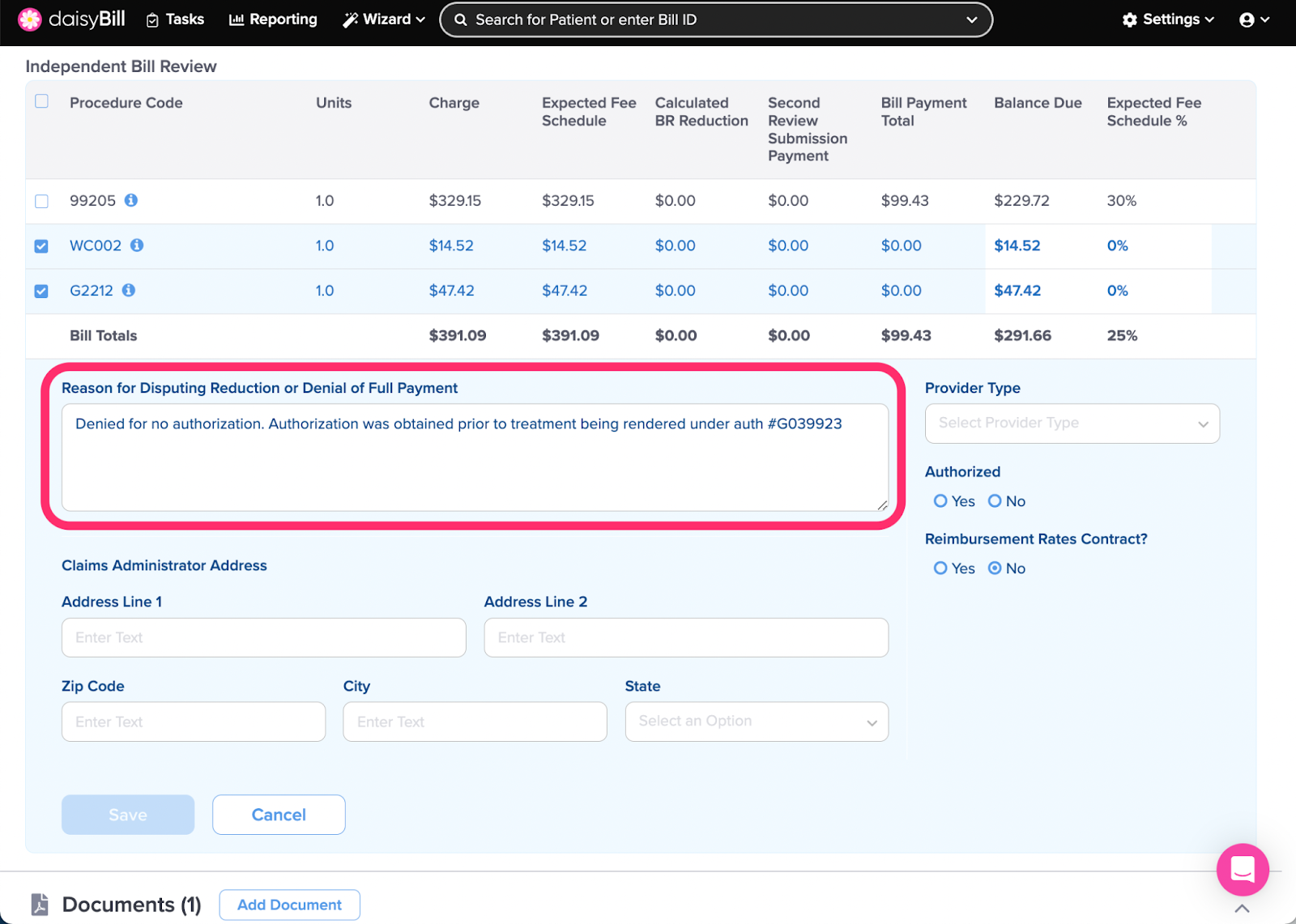
Step 3. Enter ‘Reason for Disputing Reduction or Denial of Full Payment’
This should be a concise explanation for why additional reimbursement is due on this bill. Cite labor codes and billing regulations where appropriate. The text in this field is printed directly onto the IBR-1 form.
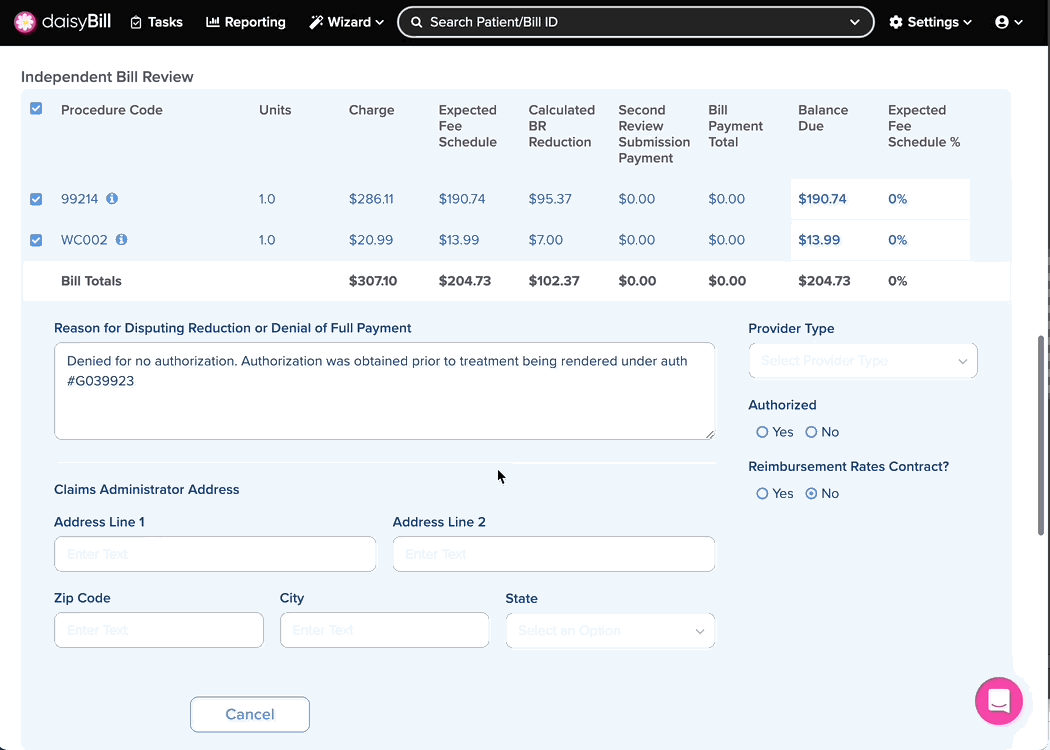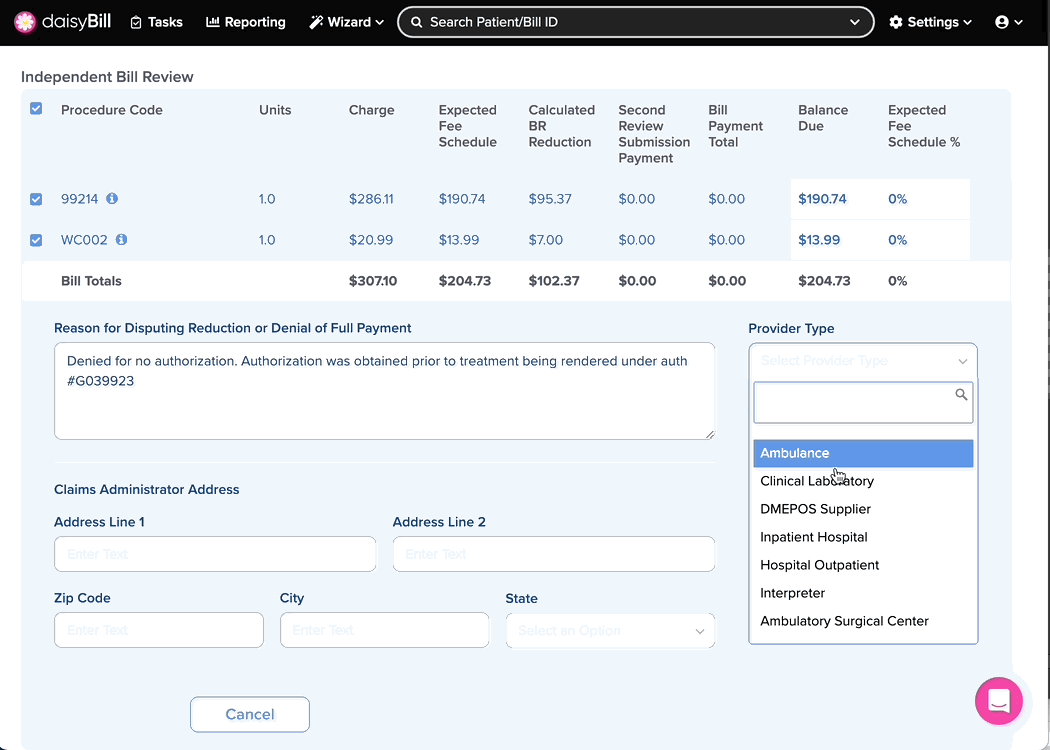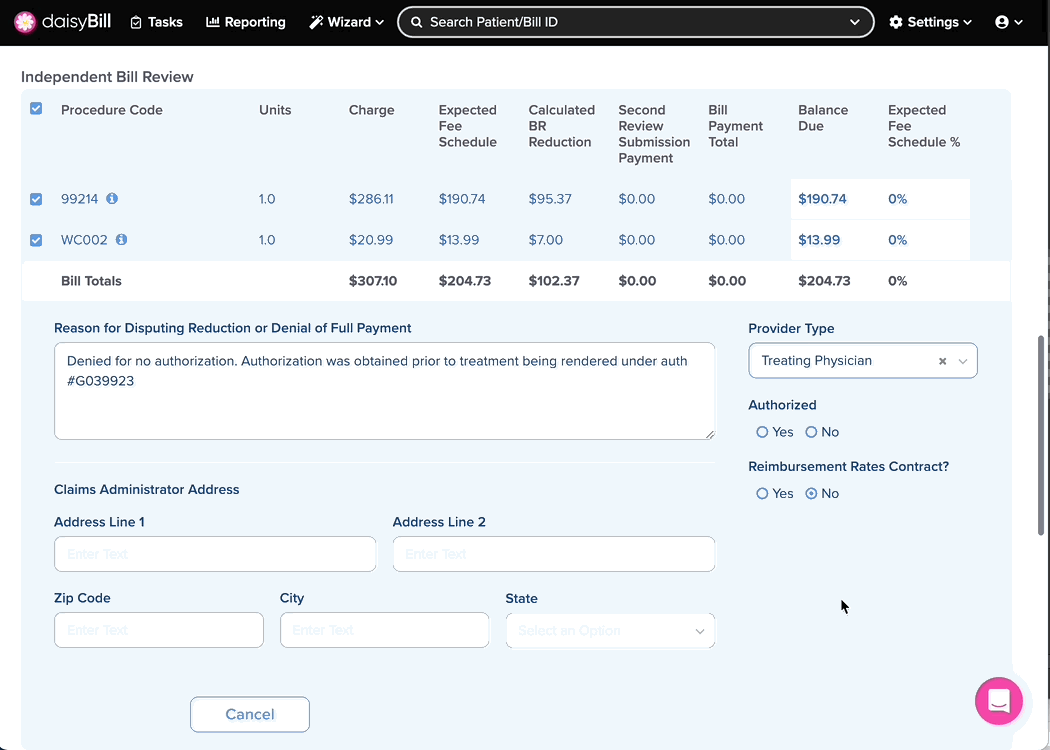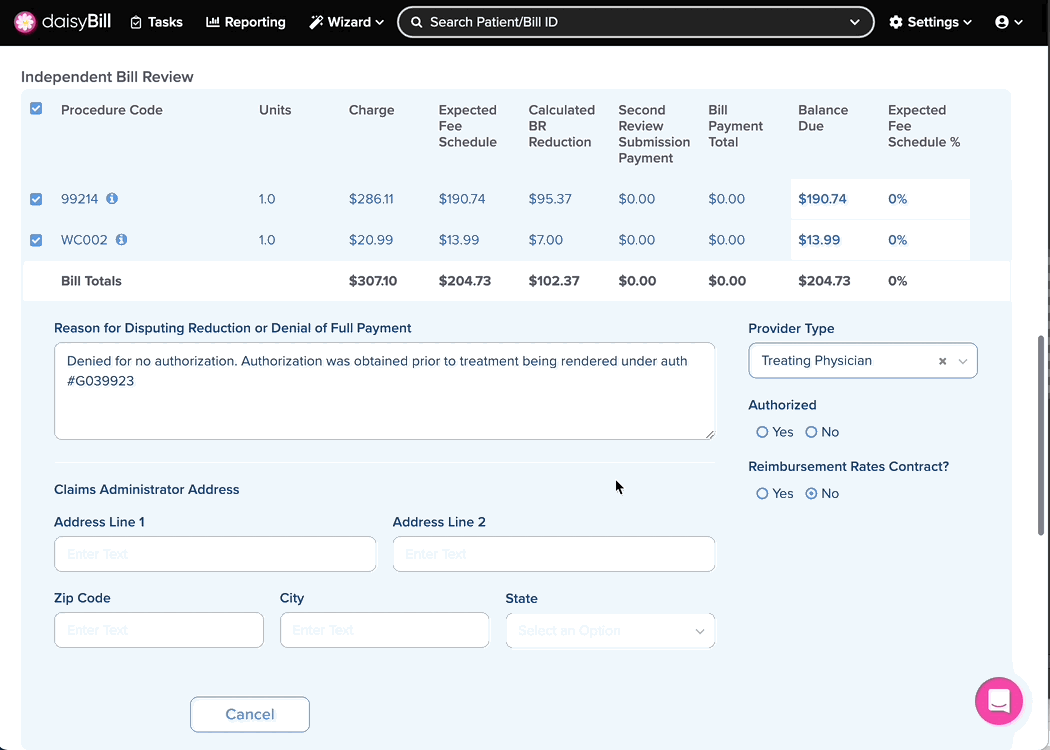
Step 4. Select ‘Provider Type’
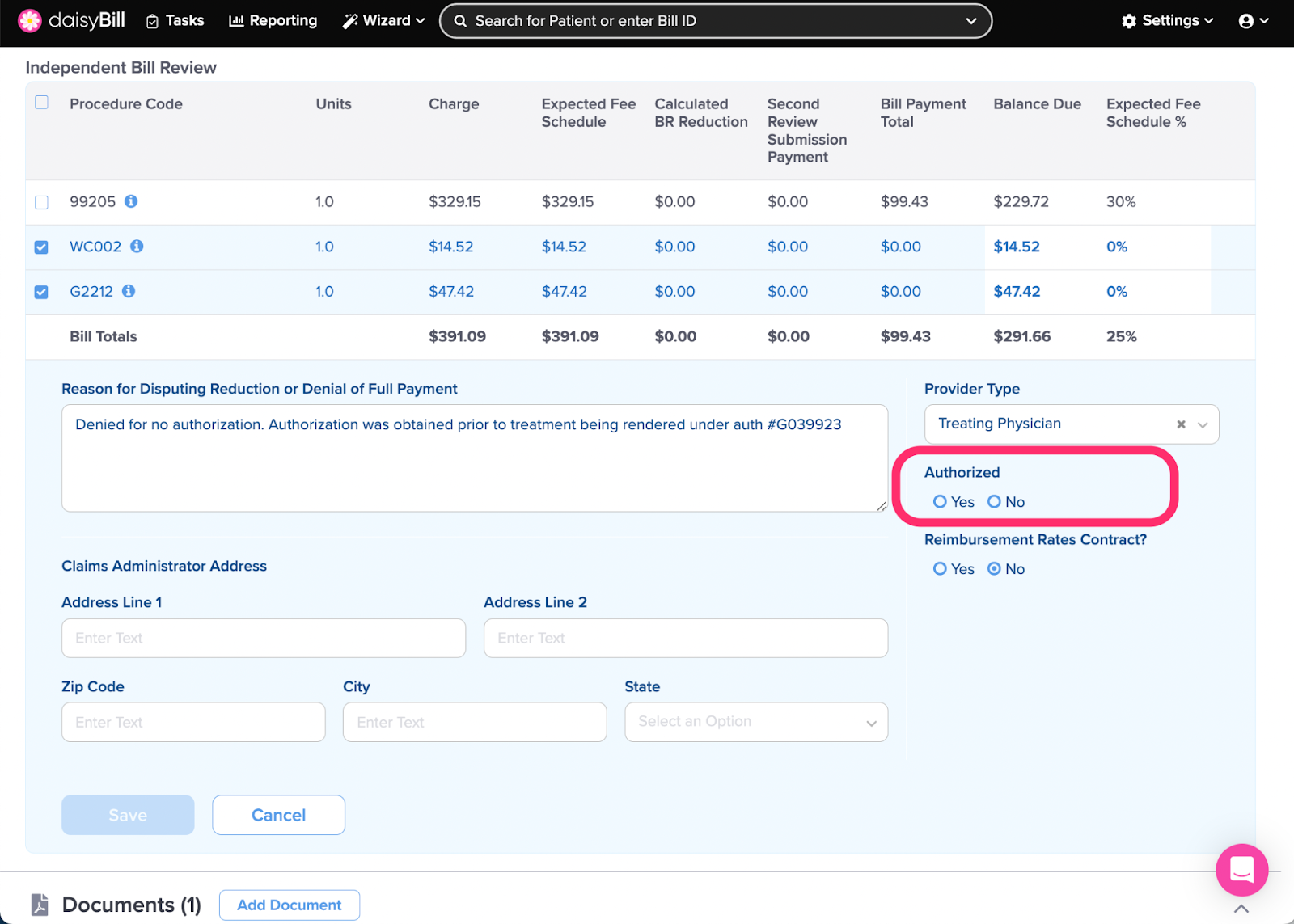
Step 5. Indicate if the Billed Service was Authorized
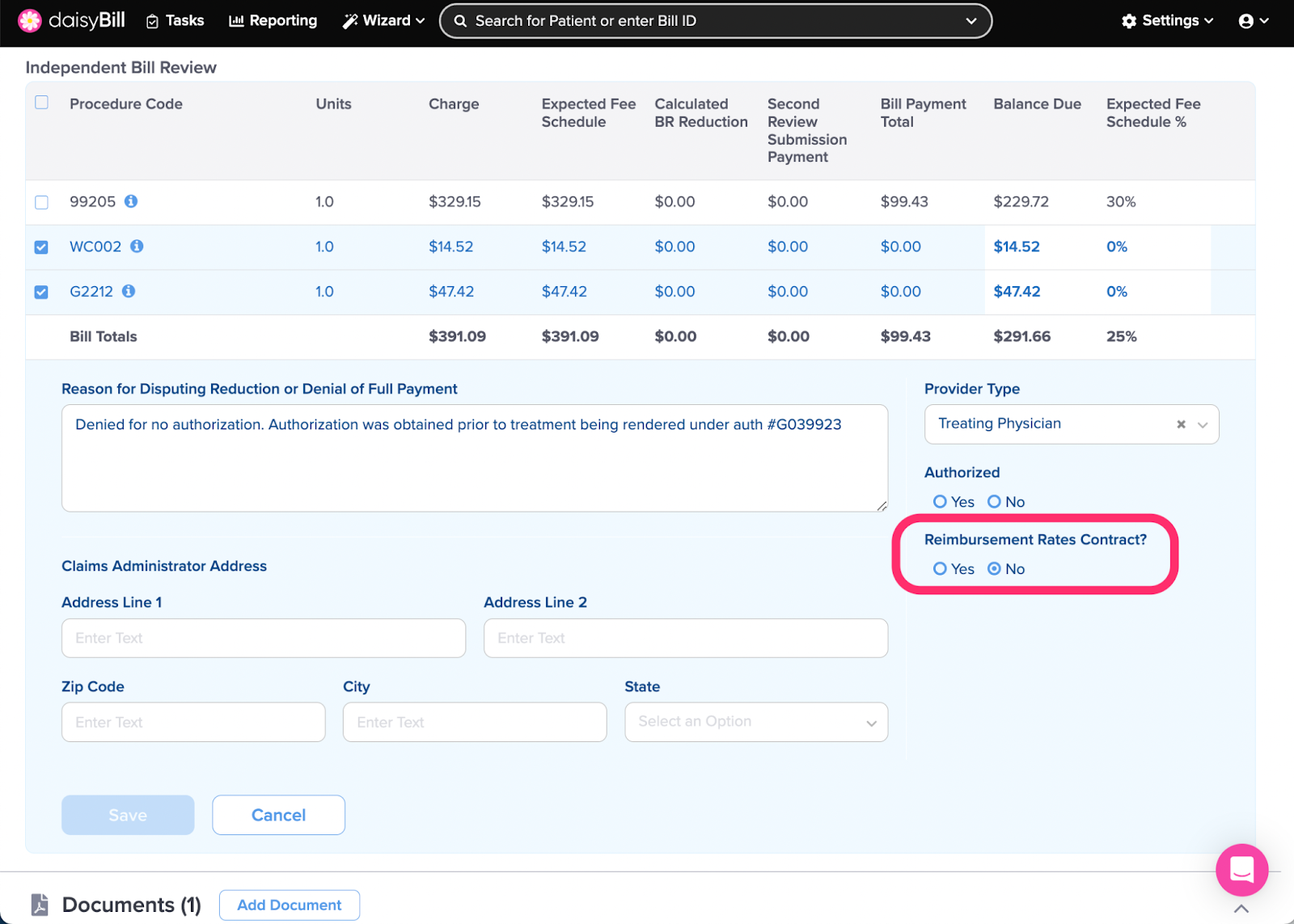
Step 6. If the Bill was processed according to a contract, select ‘Yes’ under ‘Contract for Reimbursement Rates?’ and upload ‘Relevant Contract Provisions’
- If no contractual discount was taken on the Bill, do not check the box.
- If the Bill was processed according to a network, contractual, or PPO discount check this box, even if the dispute is not about the discount.
- If Contract for Reimbursement Rates is checked, the Relevant Contract Provisions are required to be uploaded. Only the pages of the contract that summarize the reimbursement should be uploaded. Click Choose File to upload the Relevant Contract Provisions.
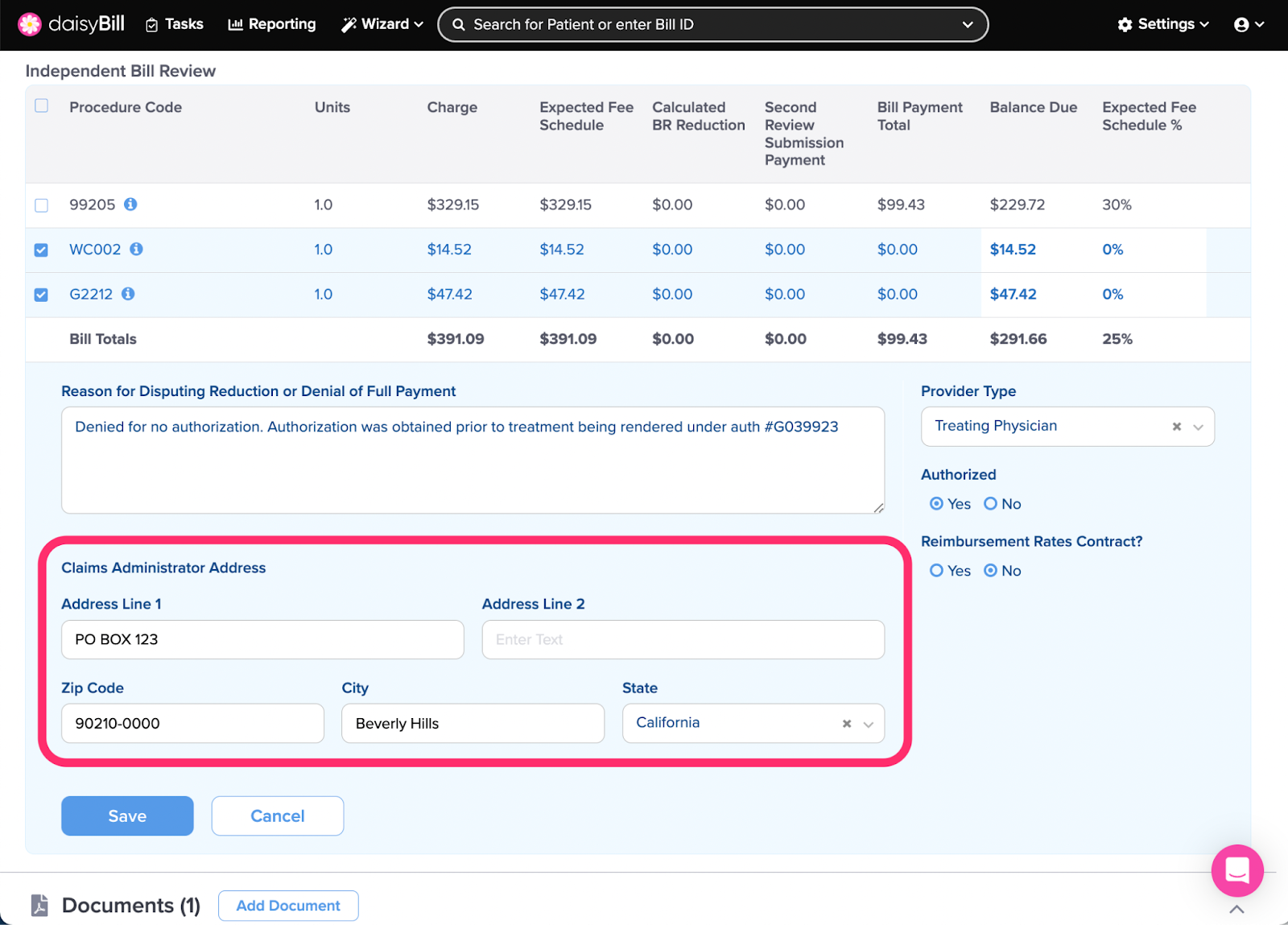
Step 7. Enter ‘Claims Administrator Address’
A copy of the IBR must be concurrently served on the claims administrator. Enter the address for the claims administrator or adjuster where the IBR should be sent. Pro Tip: Call the claims administrator and ask where IBR submissions should be sent. IBR’s can be deemed ineligible if the claims administrator is not correctly served.
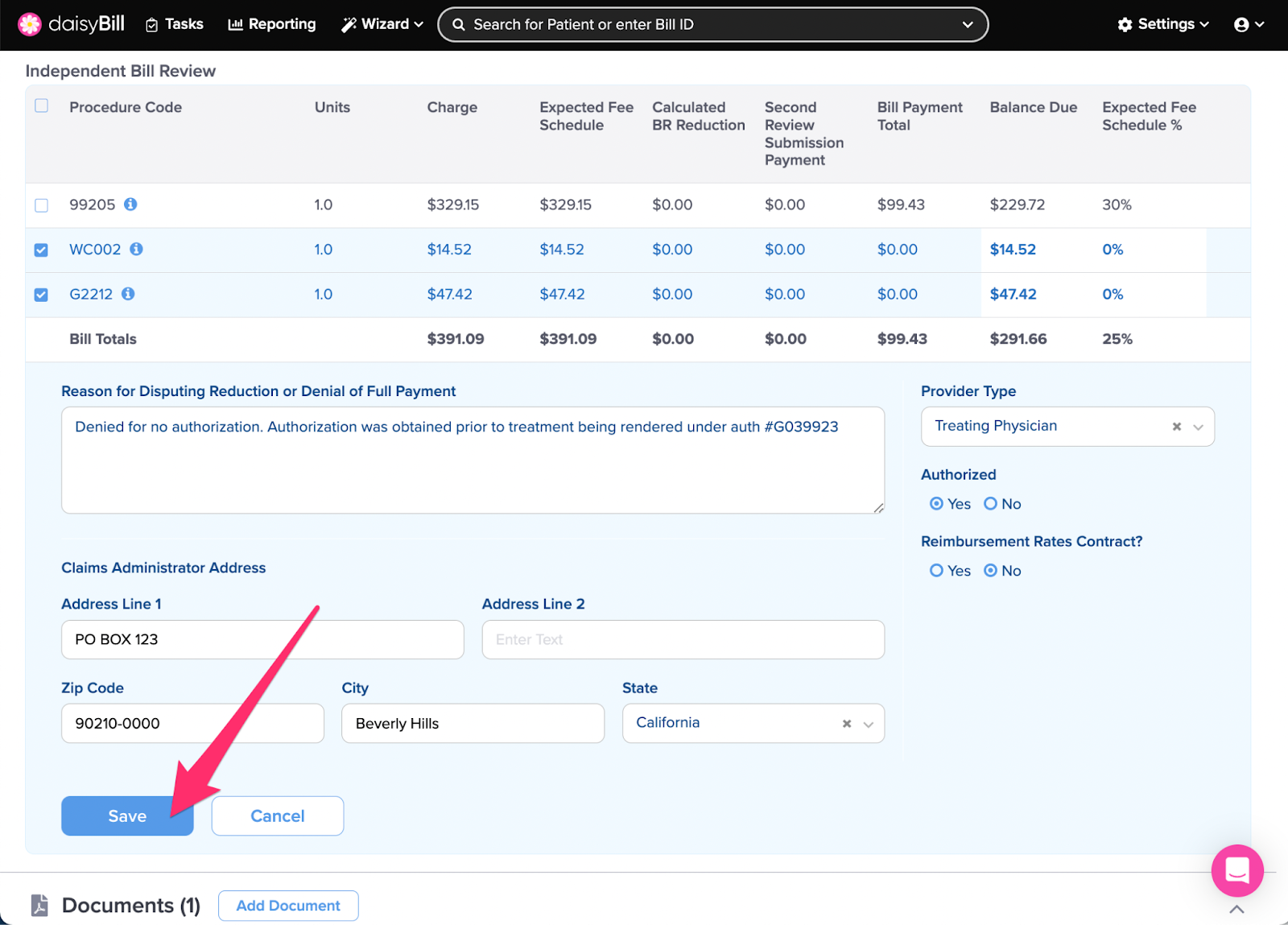
Step 8. Click ‘Save’
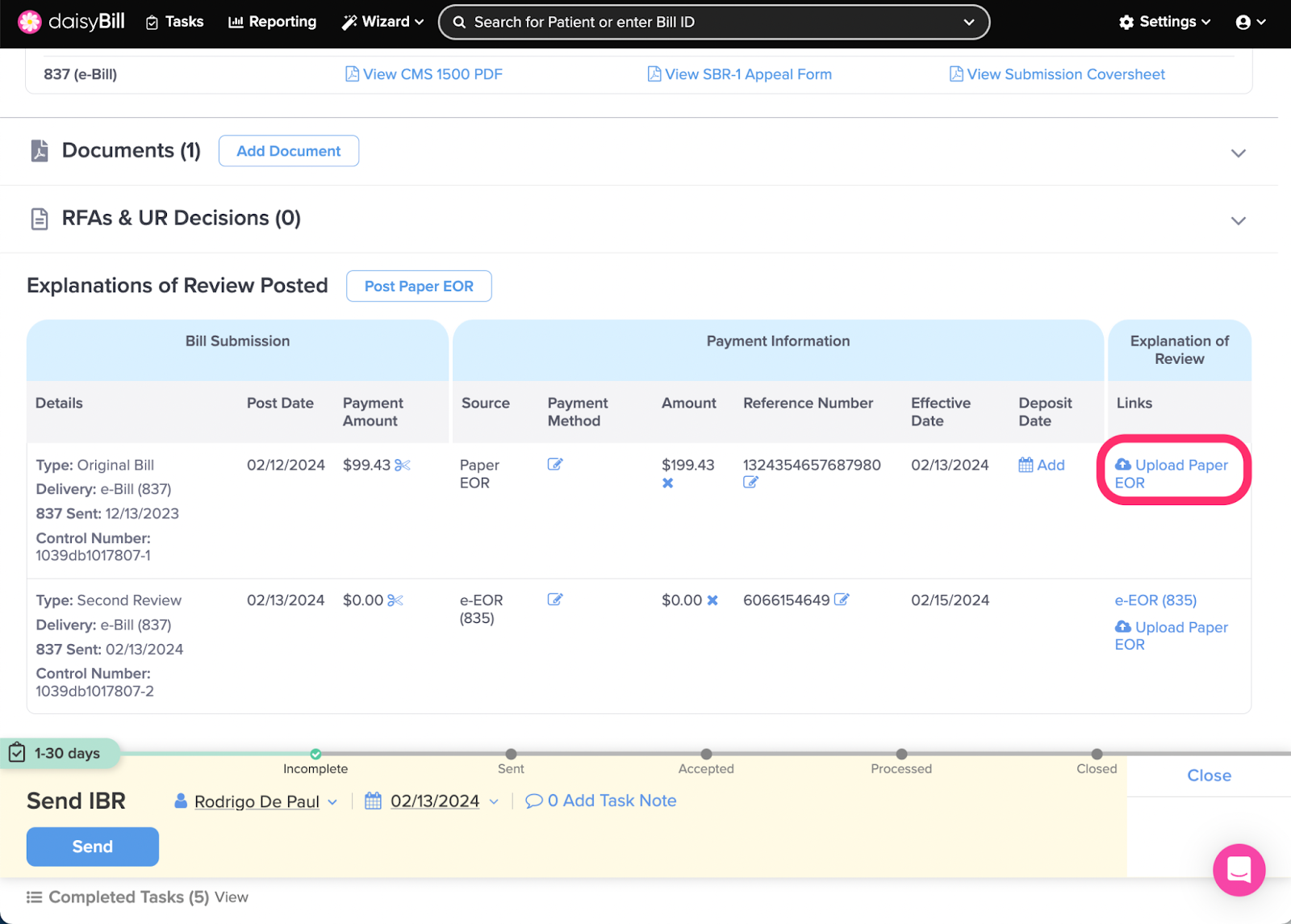
Step 9. Click the ‘Upload’ icon next to each payment and upload each paper EOR
EORs are required to create the IBR submission.
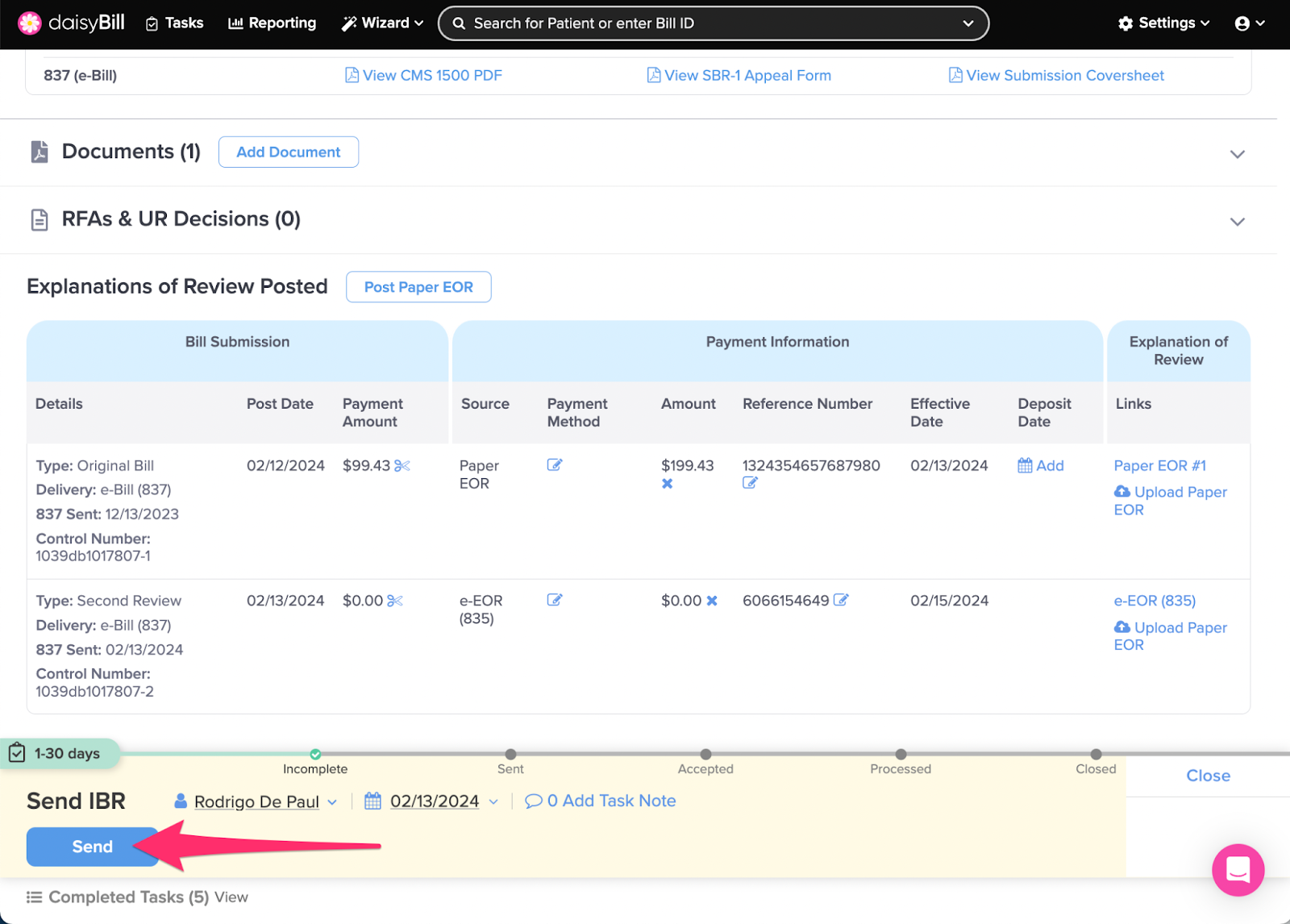
Step 10. Click ‘Send’
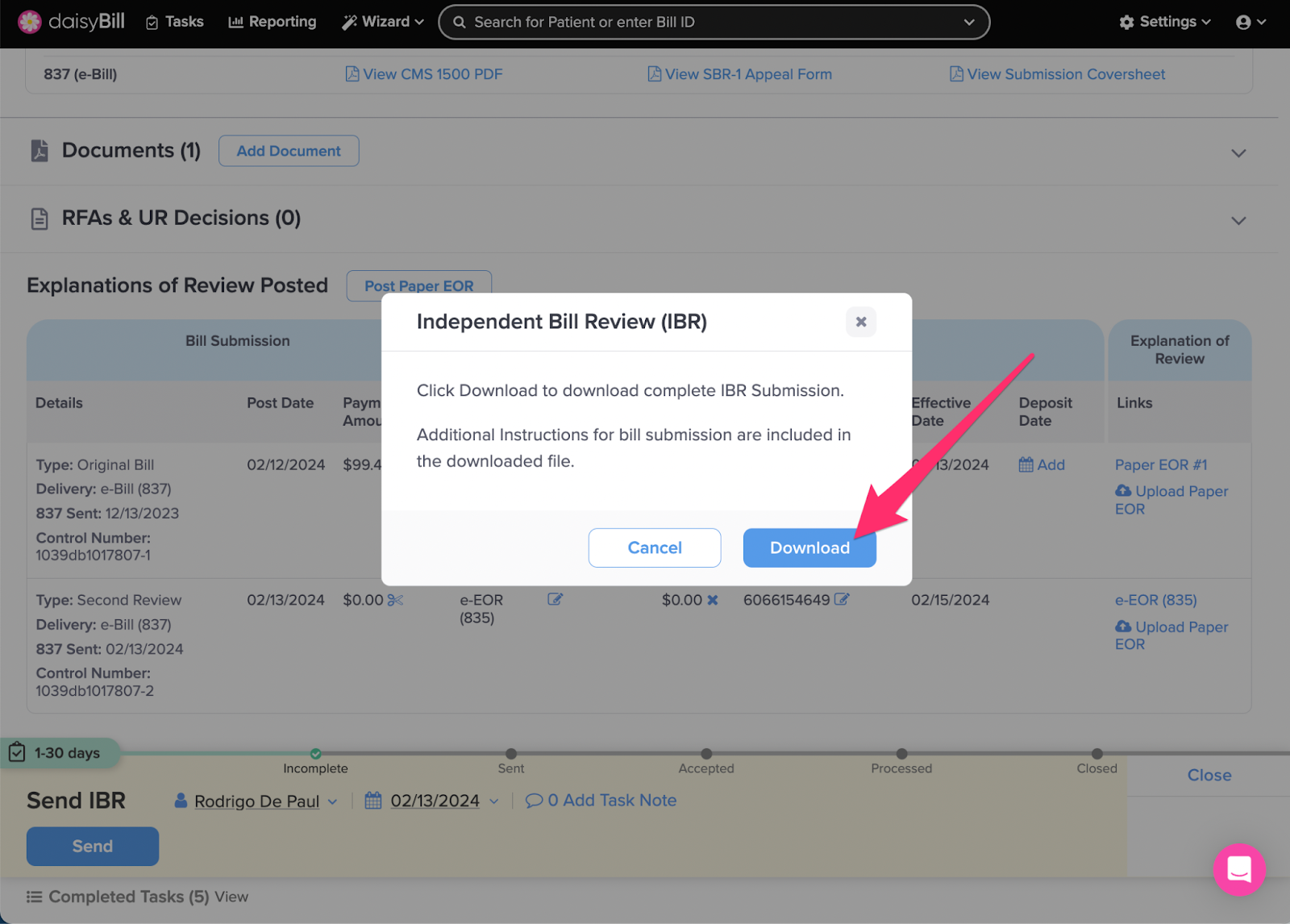
Step 11. Click ‘Download’ to create the IBR Submission
Step 12. Print the IBR Submission packet and follow the included directions page for submission
Step 13. Fill out the Proof of Service by Mail:
There are no published guidelines on how to fill out this form, but we suggest using the following guidelines indicated in red below:
You’re all set!