Summary
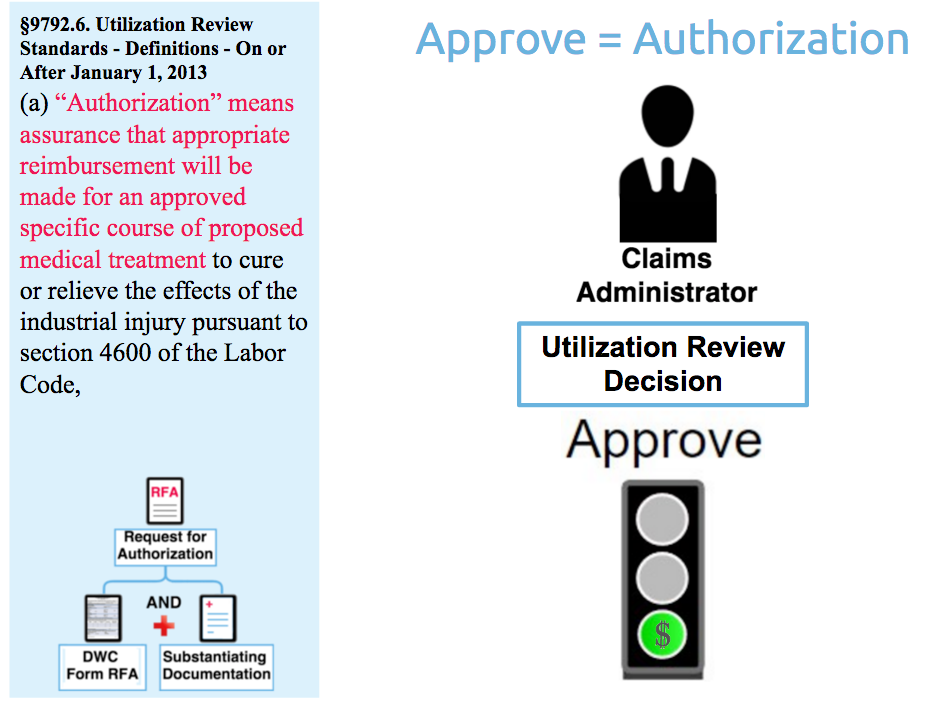
Regulation 9792.6.1, which is a list of definitions for Utilization Review, defines authorization as “assurance that appropriate reimbursement will be made for an approved specific course of proposed medical treatment...”
A utilization review decision to Approve the RFA recommended treatment guarantees the claims administrator will reimburse the requesting provider for the authorized medical services. Under the UR regulations, treatment is "authorized" when the decision to approve the RFA is communicated to the requesting physician.
Communication
Regulation 9792.9.1(d) outlines the mandatory process for communicating a utilization decision which approves the RFA requested treatment.
Regulation 9792.9.1(d)(1) requires all approve decisions to include the four elements listed below: the specific date the complete RFA was received, the medical treatment requested, the specific medical treatment approved, and the date of the decision.
For concurrent, prospective and expedited RFAs, regulation 9792.9.1(d)(2) requires the claims administrator to communicate the approve decision to the requesting physician within 24 hours of making the decision. The claims administrator must communicate the approve decision to the requesting physician via telephone, facsimile or email.
If the decision is communicated by telephone, for a concurrent review, written notice is required within 24 hours of the decision and for a prospective review within two business days.
For retrospective RFAs, regulation 9792.9.1(d)(3) requires the claims administrator to communicate the approve decision to the requesting physician who provided the medical services AND to the patient who received the medical services and to their attorney or designee if applicable. A retrospective RFA decision is due within 30 days of receipt of the RFA.
California Code of Regulations (CCR)
§ 9792.6.1 Utilization Review Standards - Definitions - On or After January 1, 2013
§ 9792.9.1 Utilization Review Standards - Timeframe, Procedures and Notice - On or After January 1, 2013
DaisyBill Resources
Daisy News: Your Request for Authorization (RFA) Questions Answered
For more information about California’s workers’ comp electronic billing, watch DaisyBill’s free, information-packed webinars.
Webinar Library