Here's the basics:
Reimbursement for dispensed pharmaceuticals is governed by the Pharmaceutical Fee Schedule as set forth in Section 9789.40 of the Labor Code.
See this FAQ for finding the Pharmaceutical Fee Schedule.
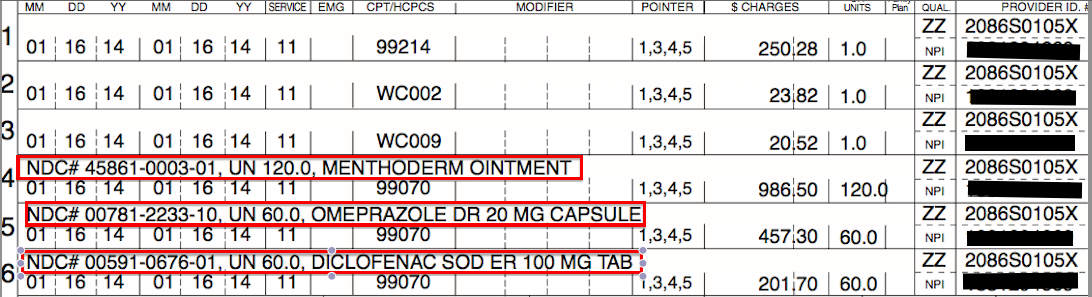
Use CPT/HCPCS code 99070 when billing for office-dispensed pharmaceuticals.
Insert the 11 digit NDC number in the supplemental field
Be sure to include the number of units so the pharmaceutical reimbursement is accurately calculated (in grams, ml, CCs, etc.)
The fee schedule amount is 100% of the Medi-Cal amount PLUS the dispensing fee of $7.25.
Only one dispensing fee is payable per drug, NOT per dispensed bottle of pills.
Pro-tip: Though not required by DWC billing regulations, daisyBill includes the name of the pharmaceutical associated with the NDC numbers. Claims administrators alerted us that the name helps them more efficiently process pharmaceutical billing.