Summary
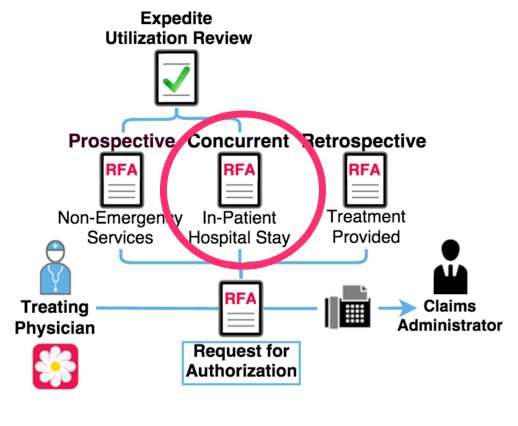
Treating physicians are required to submit a complete and compliant Request for Authorization (RFA) for treatment.
There are three RFA types: concurrent, prospective, and retrospective.
Regulation 9792.6.1 defines a concurrent review as utilization review conducted during an inpatient stay. So that a claims administrator can conduct concurrent utilization review of the requested medical services for service provided during an inpatient stay, a treating physician must submit a concurrent RFA during the inpatient stay.
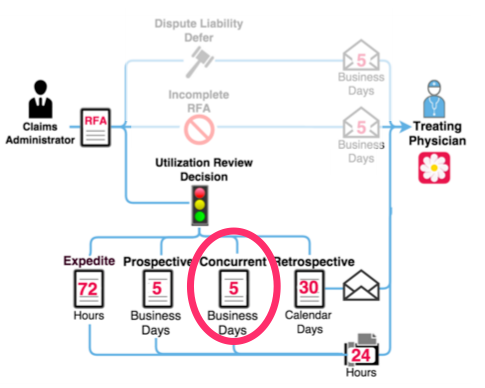
Concurrent Review Required Timeline
Per regulation 9792.9.1(c)(3), a utilization review decision for a concurrent RFA is due within 5 business days after receipt of the completed DWC Form RFA.
For a concurrent RFA, the claims administrator must communicate the decision to the requesting physician within 24 hours of making the decision. Regulation 9792.9.1(e)(3) requires the communication of the modify, delay, or deny decision to be via telephone, facsimile, or email.
Concurrent Review Penalty
If a claims administrator fails to respond to a concurrent RFA, regulation 9792.12(a) mandates that the mandatory penalty is $2,000 for each failure.
California Code of Regulations (CCR)
§ 9792.6.1 Utilization Review Standards - Definitions - On or After January 1, 2013
§ 9792.9.1 Utilization Review Standards - Timeframe, Procedures and Notice - On or After January 1, 2013
§ 9792.12 Administrative Penalty Schedule for Labor Code § 4610 Utilization Review Violations
DaisyBill Resources
Daisy News: Your Request for Authorization (RFA) Questions Answered
For more information about California’s workers’ comp electronic billing, watch DaisyBill’s free, information-packed webinars.
Webinar Library