Summary
A utilization review decision approves, modifies, delays, or denies the RFA recommended treatment.
Regulation 9792.6.1, defines utilization review as “a decision pursuant to Labor Code section 4610 to approve, modify, delay, or deny, a treatment recommendation or recommendations by a physician prior to, retrospectively, or concurrent with the provision of medical treatment services.”
According to the California Supreme Court, utilization review is required for every medical treatment requested for workers’ comp patients.
Timeframes
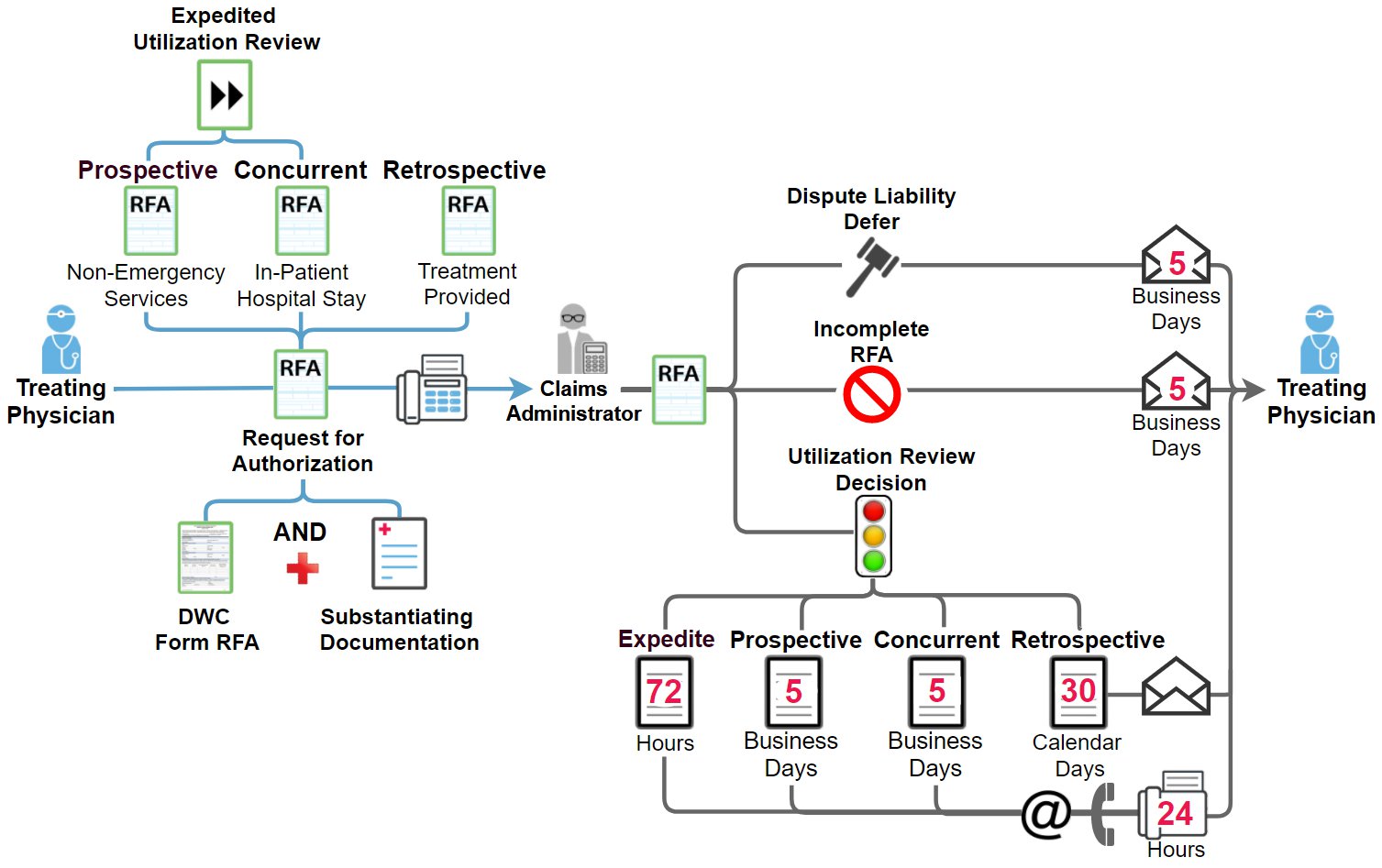
Per regulation 9792.9.1(c), the rules for calculating the required timeframes are dependent on whether the utilization review decision is due in days or in hours. When the utilization review decision is due in either 5 or 30 days, the first day is the day after the receipt of the RFA. When the decision is due in 72 hours, the first hour is the hour after the receipt of the RFA.
The DWC outlines specific timelines for UR decisions. These regulations are outlined in regulation 9792.9.1 and summarized in the workflow below.
These timelines are not optional. In Dubon II and Bodam, the Workers’ Compensation Appeals Board emphasized the importance of observing RFA timelines. The WCAB decided that:
- An untimely workers' compensation Utilization Review Decision is an invalid decision, and also that
- Claims administrators must make timely RFA decisions and must communicate RFA decisions in a timely manner.
When a provider submits a request for authorization for treatment, the regulations clearly outline the timelines for a required utilization review decision.
California Code of Regulations (CCR)
§ 9792.6.1 Utilization Review Standards - Definitions - On or After January 1, 2013
§ 9792.9.1 Utilization Review Standards - Timeframe, Procedures and Notice - On or After January 1, 2013
DaisyBill Resources
Daisy News: Your Request for Authorization (RFA) Questions Answered
For more information about California’s workers’ comp, watch DaisyBill’s free, information-packed webinars.
Webinar Library