Summary
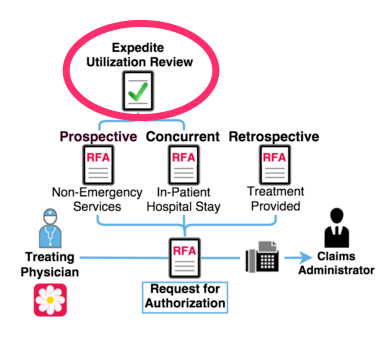
For both concurrent and prospective Requests for Authorization (RFAs), a treating physician can request that a claims administrator expedite the utilization review of the requested medical services.
If any of these four listed conditions is true, a treating physician can request an Expedited Utilization Review decision:
- If the injured worker faces an imminent and serious threat to their health, or
- the potential loss of life, limb or other major bodily function
- the normal decision making timeframe could be detrimental to the workers’ life or health, or
- the normal decision making timeframe could jeopardize the injured worker's permanent ability to regain maximum function.
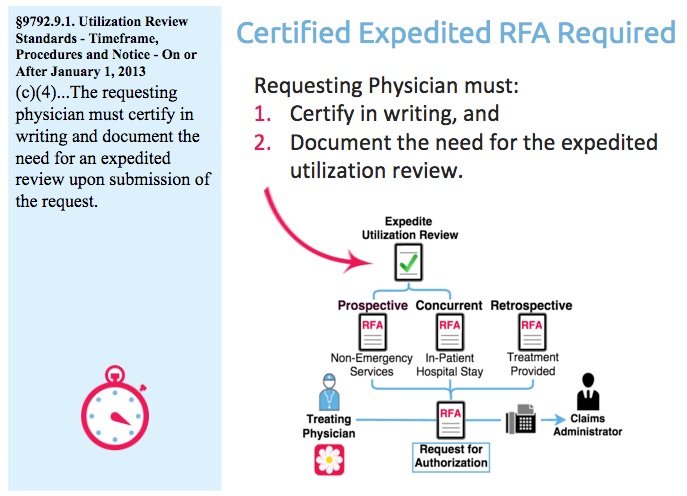
For an expedited RFA, regulation § 9792.9.1(c)(4) requires the requesting physician to “certify in writing and document the need upon submission of the request.”
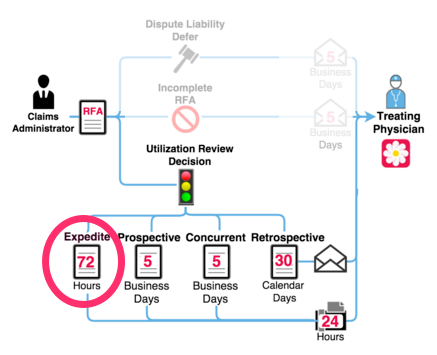
Expedited Review Required Timelines
Regulation § 9792.9.1(c)(4) requires a utilization review decision for an Expedited Prospective or Concurrent RFA within 72 hours after receipt of the “written information reasonably necessary to make the determination.” For an expedited RFA, the regulation does not require a completed DWC Form RFA.
Expedited Utilization Review Penalty
If a claims administrator fails to timely communicate the decision for an expedited RFA, regulation 9792.12(a) mandates that the mandatory penalty is $15,000 for each failure.
California Code of Regulations (CCR)
§ 9792.6.1 Utilization Review Standards - Definitions - On or After January 1, 2013
§ 9792.9.1 Utilization Review Standards - Timeframe, Procedures and Notice - On or After January 1, 2013
§ 9792.12 Administrative Penalty Schedule for Labor Code § 4610 Utilization Review Violations
DaisyBill Resources
Daisy News: Your Request for Authorization (RFA) Questions Answered
For more information about California’s workers’ comp, watch DaisyBill’s free, information-packed webinars.