§ 9789.16.4 Surgery - Global Fee; Exception: Circumstances Allowing E&M Code During the Global Period; Primary Treating Physician's Progress Report (PR-2)
Summary
For surgical codes subject to the workers' comp global period, the physician may be reimbursed for providing E&M (Evaluation and Management) services in certain circumstances. Those E&M services must be in excess of the total number of E&M visits listed for the surgical code in Section 9789.16.4, and only medically necessary E&M services in excess of that number may be separately billed.
Here are the steps to correctly calculate reimbursement for DWC’s Medicare ground rule exception:
- In the physician time file, which is in section 9789.19, find the primary procedure code being performed.
- Add up all the number of visits in the row of that procedure.
- If the total is a half number, round up.
- If the number of visits provided in the global period exceeds this number, the number of visits in excess is payable.
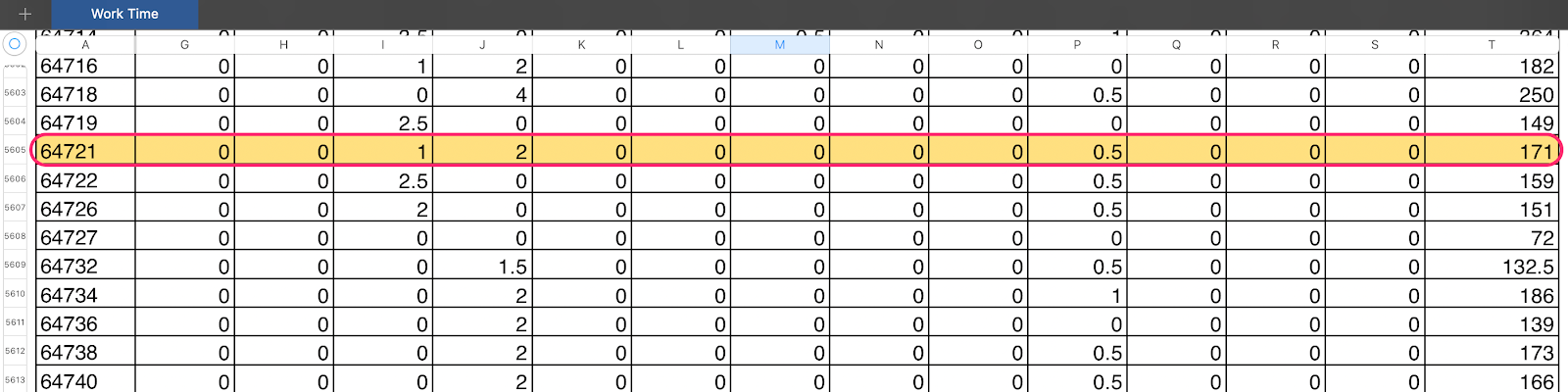
Example: Procedure Code 64721
In this example, a physician performs a carpal tunnel surgery and bills procedure code 64721.
1. Look in the physician time file.
2. Add up all the numbers in the row, which in this case is 1 + 2 + .5 which equals 3.5.
3. Since it’s a half number, round up to 4.
4. If the physician provides more than 4 medically necessary E&M visits to the patient during the global period, visits in excess of 4 are not payable.
So, if 6 visits are provided during the global period, only 2 are payable.
Keep in mind that if pre-op visits occurred, they count for surgical codes with "090" in Global Days.
What does "medically necessary" mean in the context of the global period?
Medically necessary services are those services which are typically included in the global surgical package and are therefore not payable during the Global Period.
According to Medicare ground rules these services are NOT payable during the pre and post op global periods for surgical codes; in other words, these medically necessary services are considered to be included in the global surgical package.
This is a list of medically necessary services:
- Preoperative visits after the decision is made to operate
- Major procedures: beginning the day before
- Minor procedures: beginning the day of surgery
- Intra-operative services that are normally a usual & necessary part of a surgical procedure
- Complications following surgery that don’t require a trip to the operating room
- Post-op visits related to recovery from surgery
- Post surgical pain management (by surgeon)
- Supplies (except those specifically excluded)
- Miscellaneous Services
PR-2 Reports
Section 9789.16.4(b) states that Primary Treating Physician's Progress reports (or PR-2 reports) are separately reimbursable even if the change in the patient's condition or treatment occurs during the surgical global follow-up period.
California Code of Regulations (CCR)
Division of Workers’ Compensation Websites
DaisyBill Solution
Technology is your friend when it comes to calculating correct fee schedule reimbursements. DaisyBill’s OMFS Calculator makes determining accurate reimbursements quick and hassle-free for current AND past dates of service.
Sign up for the DaisyBill Work Comp Wizard and instantly start billing easier. Click below for a FREE three day trial and start easy calculations today.
Try the DaisyBill
OMFS Calculator